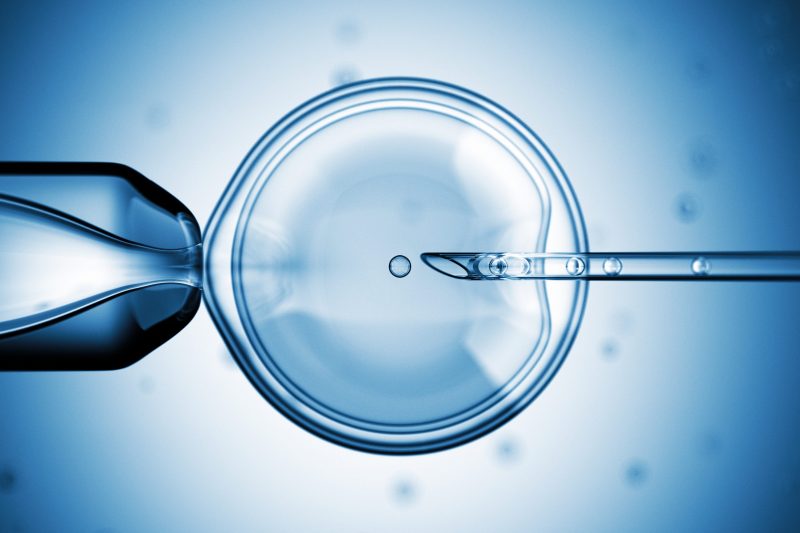
How do we know the embryos created in an IVF cycle are normal before we transfer them to the uterus? The simple answer is, we really don’t.
The likelihood an embryo will successfully implant is about 46% for women under age 35, according to national averages from over 400 IVF clinics in the U.S. For women within ages 38 to 40, those implantation chances drop to 28% and at ages 41 to 42, less than 18% of embryos will successfully implant. With increasing age, miscarriage rates also increase.
There are three potential criteria that embryologists can use to assess embryo quality, and to help physician colleagues maximize IVF success:
How do we know the embryos created in an IVF cycle are normal before we transfer them to the uterus? The simple answer is, we really don’t.
The likelihood an embryo will successfully implant is about 46% for women under age 35, according to national averages from over 400 IVF clinics in the U.S. For women within ages 38 to 40, those implantation chances drop to 28% and at ages 41 to 42, less than 18% of embryos will successfully implant. With increasing age, miscarriage rates also increase.
There are three potential criteria that embryologists can use to assess embryo quality, and to help physician colleagues maximize IVF success:
What Determines A Normal Embryo?
“My embryos were normal, but I didn’t get pregnant.” It’s one of the most common statements we hear from many of our patients who come to us for second or third opinions.
 How do we know the embryos created in an IVF cycle are normal before we transfer them to the uterus? The simple answer is, we really don’t.
The likelihood an embryo will successfully implant is about 46% for women under age 35, according to national averages from over 400 IVF clinics in the U.S. For women within ages 38 to 40, those implantation chances drop to 28% and at ages 41 to 42, less than 18% of embryos will successfully implant. With increasing age, miscarriage rates also increase.
There are three potential criteria that embryologists can use to assess embryo quality, and to help physician colleagues maximize IVF success:
How do we know the embryos created in an IVF cycle are normal before we transfer them to the uterus? The simple answer is, we really don’t.
The likelihood an embryo will successfully implant is about 46% for women under age 35, according to national averages from over 400 IVF clinics in the U.S. For women within ages 38 to 40, those implantation chances drop to 28% and at ages 41 to 42, less than 18% of embryos will successfully implant. With increasing age, miscarriage rates also increase.
There are three potential criteria that embryologists can use to assess embryo quality, and to help physician colleagues maximize IVF success:
 How do we know the embryos created in an IVF cycle are normal before we transfer them to the uterus? The simple answer is, we really don’t.
The likelihood an embryo will successfully implant is about 46% for women under age 35, according to national averages from over 400 IVF clinics in the U.S. For women within ages 38 to 40, those implantation chances drop to 28% and at ages 41 to 42, less than 18% of embryos will successfully implant. With increasing age, miscarriage rates also increase.
There are three potential criteria that embryologists can use to assess embryo quality, and to help physician colleagues maximize IVF success:
How do we know the embryos created in an IVF cycle are normal before we transfer them to the uterus? The simple answer is, we really don’t.
The likelihood an embryo will successfully implant is about 46% for women under age 35, according to national averages from over 400 IVF clinics in the U.S. For women within ages 38 to 40, those implantation chances drop to 28% and at ages 41 to 42, less than 18% of embryos will successfully implant. With increasing age, miscarriage rates also increase.
There are three potential criteria that embryologists can use to assess embryo quality, and to help physician colleagues maximize IVF success:
Subscribe to stay in the loop
Our newsletter delivers expert insights, practical benefit strategies, heart warming member
moments, and the latest in fertility and family-building news straight to your inbox.